Information AboutTelogen Effluvium and Its Causes
Telogen Effluvium -Ken Washenik, MD, PhD
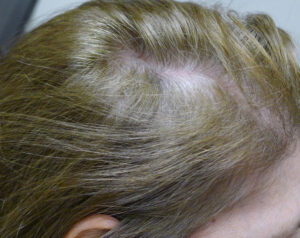
Telogen Effluvium
See FAQs at the bottom of the page.
Telogen is the last of the three stages in the hair growth cycle. After growing in the anagen stage, hair enters a short transition stage, catagen, before reaching telogen. Telogen is often described as the resting stage. At the end of the telogen stage, the hair shaft falls out (the actual shedding of the hair shaft has recently been named exogen and is described in an article on exogen by Dr. Kurt Stenn on this website) and the cycle starts over again.
Telogen hairs are the hairs that are routinely shed throughout the day and are most often noted while washing or brushing your hair. Approximately one out of every ten scalp hairs are normally in telogen. Shedding fifty to one hundred telogen hairs per day is considered normal. Losing more hairs than that is referred to as a telogen effluvium. It occurs when an increased number of hairs (i.e., more than one in ten) are in the telogen stage of the hair growth cycle. This abrupt shift of anagen hairs into telogen results in increased shedding several (approximately three) months later since that is the length of time hairs stay in the telogen stage prior to falling out.
A telogen effluvium may be caused by a number of factors. Depending on the length of time this increased shedding persists, it is referred to as an acute or chronic telogen effluvium. In an acute telogen effluvium, the shedding can persist for up to six months. When the shedding lasts more than six months, or persistently cycles in and out of periods of increased shedding, it is called a chronic telogen effluvium. A chronic telogen effluvium can last for years. Chronic telogen effluvium is more often reported in women than men. The reason for this gender difference is unknown as is the actual cause of chronic telogen effluvium in most patients.
An area of confusion concerning the diagnosis of telogen effluvium is the fact that making the diagnosis does not necessarily lead to an understanding of its cause in a particular patient. The increase in hair shedding can be caused by a fairly large number of factors. In fact, telogen effluvium is best thought of as a reaction to something rather than a particular disorder unto itself. The causes of telogen effluvium are varied and not always determinable. Common causes include childbirth or the cessation of oral contraceptives, surgery with general anesthesia, severe systemic illness including fever, thyroid disease and inadequate nutrition, especially insufficient intake of protein. A number of different medications have been implicated in the etiology of telogen effluvium. These include anticoagulants, retinoids (or excess vitamin A), lithium and beta blockers among others. The list of potentially causative drugs continues to grow.
The diagnosis of telogen effluvium can be made by a physician experienced in treating patients with hair disorders after a thorough discussion of the patient's medical history and examination of the hair and scalp. The physician may elect to perform a "hair pull test" or a biopsy of the scalp. Either or both should reveal an increase in the percentage of telogen hairs found. Telogen hairs can be identified by the small, barely perceptible hair bulb on the end of the hair. They are also referred to as club hairs.
Treatment of telogen effluvium is dictated by its cause whenever it is known. The shedding experienced after pregnancy or the cessation of oral contraceptive therapy is self limited and will resolve without treatment. An effluvium caused by a systemic illness is treated by treating the illness. Nutritional deficiencies should be corrected. If the effluvium is caused by a particular drug, the use an alternative medication should be considered. When the problematic medication is stopped, the shedding will persist for several months. (However, it is important to remember that it may not be possible to find a medically acceptable substitute for the medication causing the effluvium).
Topical minoxidil solution (two percent or five percent) is a useful treatment for a significant number of patients with chronic telogen effluvium. It is applied twice a day and exerts its effect in approximately three months. Minoxidil can be helpful as it can prolong the anagen stage of the hair cycle. Finasteride is not beneficial in treating telogen effluvium, unless it is caused by androgenetic alopecia in a male.
References:
Telogen Effluvium Frequently Asked Questions:
The following are frequently asked questions on telogen effluvium. The information provided is not meant to be a substitute for the information obtained at an evaluation and by discussion with a physician, but merely to encourage understanding of this condition. No questions regarding individual scenarios will be answered by the AHRS. No changes in treatment should be undertaken by a patient without discussion first with the patient's physician.
